The summer between MS1 and MS2 I did a research project with an orthopedic surgeon at my school. Part of the project had me observing in the operating room (OR) a few days a week, watching procedures and helping with any tasks that came up. This experience was actually my first time being in an OR, and I was pretty nervous leading up to it. I had heard horror stories about students breaking sterility, knocking over solution bottles, and generally making fools of themselves in front of important people. While I tried my best not to do anything foolish or embarrassing, it was oftentimes very hard to avoid. Slowly, I become more confident in the OR, and the blunders came further and further apart. As a service to all the pre-meds and un-initiated med students, I now present a short list of important things to know before your first OR experience.
- Figure out the rules. Surgeons love rules, and at times it seems as if they have a weird fascination with them. If you don’t ask then the rules are never really explained to you, and you will be in big trouble when you break one. Consequently, I think it’s prudent to ask someone what the rules are. Considering your fear of talking to the surgeon, he or she isn’t the best option. The resident or intern is probably too sleep-deprived and hopped-up on caffeine to notice you. Your best bet is to ask one of the circulating nurses or other students who have been on the service for a while. Believe me, it will save you a lot of trouble later on.
- Make sure you’re dressed appropriately. Make sure everything you’re supposed to wear is on correctly. Make a mental note of scrubs, cap, mask, and boots. Aside from actually wearing the right attire, please make sure you are wearing it correctly. You’re going to feel really stupid when someone points out that your cap is on crooked, or that you forgot to tie half of your mask. You will also be the butt of many jokes over the next few days when you aren’t there. In addition to knowing what to wear, it is also important to know what not to wear. Don’t wear shoes that you actually like, unless you think it’s cool to have fecal matter on your $100 Sperry’s. Also, leave the personal items and accessories at home. While that puka shell necklace you made in 10th grade art class may be “totally rad, bro,” it is definitely a sterility hazard and you definitely shouldn’t bring it into the OR. Also, if you’re still wearing puka shell necklaces in your mid-20s you should probably re-evaluate your life choices.
- Know where the sterile field is and how to avoid it. This rule only applies if you’re not scrubbed in, and the decision of whether or not you get to scrub should have decided before you show up. Anyway, just remember that the sterile field should be avoided like the plague. Any blue towel or covering should send off warning signals in your head. Don’t get close to it, don’t breathe on it, and don’t even really look at it if you don’t have to. Don’t try to be cute either and inch your way as close as possible, because the scrub nurse will call you out and you will be embarrassed.
- Try to look interested even when you’re not. After the 5th time seeing the same surgery, it’s only human nature to get a little disinterested. There are only so many times you can be mystified by a hernia repair, and you’ve probably passed that threshold long ago. It is imperative, however, that you look interested at all times. Surgeons have an innate ability, almost like boredom-radar, to tell when you are dozing off or doing something else. These situations usually end up in you getting pimped mercilessly in front of everyone. To make matters worse, you don’t come off looking like a shining star when your response to the first question is “Huh?” You can typically avoid these situations by employing certain maneuvers that indicate “interest.” My go-to method was switching sides of the OR every 20 minutes to get a new “viewing-angle.” Another tried and tested one is intently looking at the monitors or camera. Find what method works for you, and stick to it.
- If you’re not scrubbed in, find yourself a role. Surgeons dislike idle people. There’s nothing worse you can do than to just stand in the same place in the OR doing nothing. Find a job you can do, and be amazing at it. Like to record information? Write down the incision and closing times. Like to clean? Become the best darn disinfectant wipe user ever. Like to retrieve things? Be the person who looks up and prints all the obscure research papers the surgeon even tangentially mentions during the procedure. Note: If you choose the last one, be prepared for incessant pimping later. Remember folks, nothing is without consequence, so choose your punishment wisely.
- Prepare yourself for the spectacle that is a patient waking-up post-op. This is the part that you never hear about or even see on those dramatized TV shows about surgery. A patient waking up from anesthesia is most definitely not pleasant. Prepare yourselves for all sorts of near disasters. Patients will try to pull out breathing tubes, or roll over onto joints that have just been operated on. Some will even try to get out of the bed, as they don’t realize where they are for the first few minutes. People will often kick out their arms and legs, and if they aren’t stabilized someone on the team is bound to get a black eye. The best thing you can do is to be aware of the possibilities, and find out how the team handles such situations.
- Find a place to store food for post-op consumption. We have finally reached the pinnacle, the crown jewel of my OR guide. Don’t pay attention to the fact that this rule actually doesn’t correspond to anything taking place in the OR. After spending countless hours in the OR, the first thing on your mind will be food. No matter how mundane or exciting the procedure was, human need for nutritional sustenance will take over. Make sure you have a safe storage spot for food, whether it is in the clinical workroom or in the students’ lounge. Also, considering that everyone you will be working with (read: vultures) will also be voraciously hungry and will have no problem eating anything lying around, make sure you keep your food in a place only you can find it. Invest in a locker and a lock if your facilities have them. You’ll thank me for this advice later. You’re welcome, by the way.
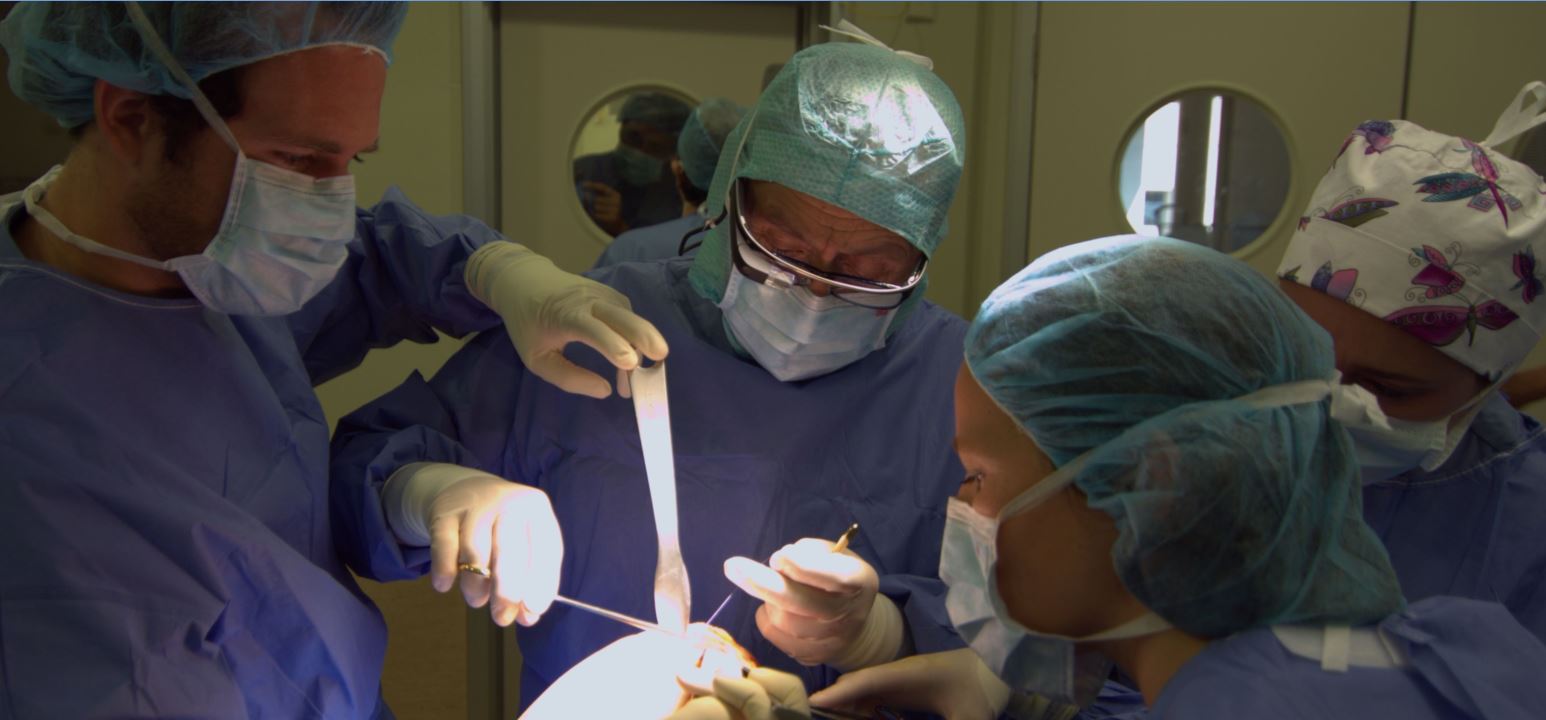
Featured image:
CPMC Surgery by Artur Bergman